Compassionate Communities
We all know people who are facing bereavement, death, end of life or significant loss. In such situations, people may experience loneliness, social isolation or even psychological distress. The community can make a difference in their well-being and support them through these difficult times.
The Compassionate Communities approach is based on a perspective of health promotion at the end of life, capitalizing on a synergy between the strengths of the community and the health system. In a co-construction approach, community organizations, citizen groups, workplaces, schools and faith groups are invited to identify their own needs related to bereavement, end-of-life and significant losses and to define the solutions they deem appropriate to meet them.
Instigated by the Palliative Care Institute of Montreal and the Canada Research Chair on Partnerships with Patients and the Public, this 5-year action-research project aims to co-construct, implement and evaluate two compassionate communities, one in the Centre-Sud neighborhood and the other in West-Island area of Montreal.
This project catalyzed the creation of Compassionate Community Montreal, a not-for-profit organization fostering engagement of communities and civil society with aging, significant loss, dying and grief.
Current Initiatives
Montréal, Qc, Canada
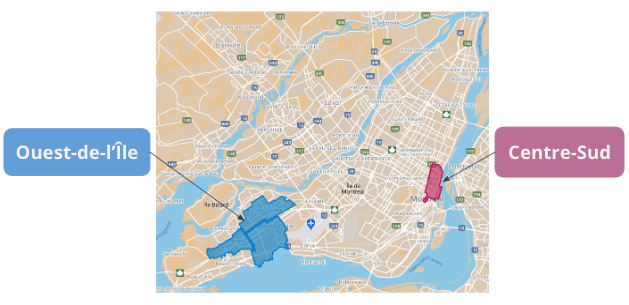
West-Island
Nav-CARE In-Home Support Program
In October 2021, Teresa Dellar Palliative Care Residence began implementing the Nav-CARE program, which was first developed in Western Canada. This program allows volunteers to provide in-home support to seniors who are living with chronic illness, social isolation, or to exhausted caregivers. The goal is to provide emotional support to seniors whose health is declining and to facilitate access to health care professionals in order to improve their quality of life. About ten trained volunteers have been matched with fifteen seniors from the West Island of Montreal. Other volunteers are currently being trained to offer Nav-CARE services. Partnerships with various community organizations, municipalities and seniors’ residences will allow them to recruit and train more volunteers and to reach more seniors in need of home support in the West Island.
More information on the program or to become a volunteer

Advance Care Planning Sessions
The Teresa Dellar Palliative Care Residence is offering free educational sessions on Advance Care Planning. The goal is to educate citizens or representatives of community organizations about the importance of thinking about and planning for health care in the event that individuals are no longer able to do so due to deteriorating health. Session content is based on best practices in advance care planning, and has been developed with Canadian experts. Training is available to support volunteer facilitators and anyone with experience in presenting, facilitating or teaching or who has a passion for advance care planning and desires to pass it on.
Thanks to the Compassionate Community project, Advance Care Planning sessions have been enhanced and tailored to the needs of the individuals reached by community partners. For example, sessions were offered in partnership with the Alzheimer Group Inc (AGI) and Kirkland and Dollard-des-Ormeaux public libraries.
Centre-Sud
Forum Citoyen 2023
In May 2023, nearly 50 members from Montreal’s Centre-Sud community (citizens, members of community organizations, municipal and provincial elected officials, researchers and healthcare professionals) gathered to discuss emerging compassionate community initiatives in the neighborhood. They also mobilized around priority actions and themes for their community (e.g. non-standard bereavement, advance planning, compassionate vigil, arts and rituals, intergenerational projects).
The compassionate community concept is based on shared interests and deserves to be better known and more widely disseminated, as it enables us to build community across differences.
For any questions or initiatives, please contact Lise Jean : ljean.compassioncsud@gmail.com.
Grieving and death cafes
Consultation meetings conducted in winter 2021 with community organizations allowed to identify a need to discuss the deaths and grief experienced by community workers. Some discovered residents who had died alone in their apartments, others had to identify them once found by emergency services. Thanks to the partnership and expertise of volunteers from the PalliAmi Foundation and a community organizer from the Association québécoise pour la promotion de la santé des personnes utilisatrices de drogues (AQPSUD), death cafés were offered to community organization workers in the Centre-Sud neighbourhood in the spring and summer of 2022. These discussion workshops provided a space for workers to talk about the deaths of users in their organizations, and initiated support of those who are dealing with unresolved grief.
The partnership between the PalliAmi Foundation and the AQPSUD was then extended to the organization Mom’s Stop the Harm, which led to the grief discussion groups for people who have experienced the loss of a loved one by overdose, who are often confronted with the prejudices and stigma that weigh on people who use drugs.


COMPAS project of Mission Bon Accueil
Implemented in the winter of 2022, the COMPAS project is a telephone monitoring program, which was created in response to the concerns about social isolation and vulnerability of the Mission Bon Accueil users, particularly seniors, reached by the organization’s food bank delivery service. The COMPAS project was set up to promote the social integration of seniors in the community, to ensure access to health and social services adapted to their needs, and to initiate a conversation with users and their families about end-of-life. Thanks to the Compassionate Community project, the organization’s representatives were supported and accompanied throughout the development and implementation of the project.

Publications
Lessard, É., O’Brien, N., Panaite, AC., Leclaire, M., Castonguay, G., Rouly, G., Boivin, A. Can you be a peer if you don’t share the same health or social conditions? A qualitative study on peer integration in a primary care setting. BMC Prim. Care 25, 298 (2024). https://doi.org/10.1186/s12875-024-02548-5
Lessard, É., Marcoux, I., Daneault, S., Panaite, A. C., Jean, L., Talbot, M., Weil, D., Rouly, G., Sallnow, L., Kellehear, A., & Boivin, A. (2023). How does community engagement evolve in different compassionate community contexts? A longitudinal comparative ethnographic research protocol. Palliative care and social practice, 17, 26323524231168426. https://doi.org/10.1177/26323524231168426
Dumont, K., Marcoux, I., Warren, É., Alem, F., Alvar, B., Ballu, G., … & Boivin, A. (2022). How compassionate communities are implemented and evaluated in practice: a scoping review. BMC Palliative Care, 21(1), 1-13. https://doi.org/10.1186/s12904-022-01021-3
Collaborations
Pallium Canada, BC Centre for Palliative Care and Hospice Palliative Care Ontario. (2023). Evaluation Guide for Compassionate Communities. Canada.
[Order a copy]
Conference Presentations
Lessard, É. (2022). Developing Compassionate Communities: Building on Community Needs, Strengths and Capacities. [Oral communication]. 7th Public Health Palliative Care International Conference. Bruges, Belgium.
Bostock A. 2020 virtual CHPCA Learning Institute. Canadian Hospice Palliative Care Association (CHPCA). Ottawa (Canada). November 2, 2020. Online conference.
Daneault S., Boivin A. En quoi le modèle des communautés bienveillantes peut constituer une avancée pour les soins. SFAP-FISP Congress. June 13-15, 2019. Paris (France). Oral presentation.
Daneault S., Bostock A., Weil D., Boivin A. Un projet de recherche sur les communautés bienveillantes. Curie-Sherbrooke Partnership, Interfaculty Service for Palliative and End-of-Life Care (SISPFV). Sherbrooke (Canada). February 27, 2020.
Guest Presentations
Boivin A. La communauté bienveillante – un modèle pour les soins palliatifs? 29th Annual conference of the Association québécoise de soins palliatifs (AQSP). Montreal (Canada). May 8th, 2019. Closing Plenary.
Boivin A., Rouly G. Soigner avec la communauté: Du début à la fin de la vie. Annual Day of the Chaire de la famille Blanchard pour l’enseignement et la recherche en soins palliatifs. May 28, 2019. Montreal (Canada). Oral presentation.
Rouly G (panelist). End of Life in Primary Health Care in Canada. Webinar from the Pan-Canadian Strategy for Patient-Oriented Research (SPOR) Network in Primary and Integrated Health Care Innovations (PIHCI). PIHCI Network Learning Series 2020-2021 #4. March 23th 2021. Recording available online [1h à 1h11].
Weil D, Bostock A. Mobilizing communities and stakeholders in the health care sector to increase capacity and quality of palliative care, cost effectively for the benefit of patients and their families. Presentation as part of the CPRL 223 course – Basics of Public Relations. McGill University’s School of Continuing Studies. May 28, 2019.
Weil D, Bostock A. Mobilizing communities and stakeholders in the health care sector to increase capacity and quality of palliative care, cost effectively for the benefit of patients and their families. Presentation as part of the CPRL 540 course – Communication Planning. McGill University’s School of Continuing Studies. June 4 and 25, 2019.
Media Relations: Interviews
Interview with Ghislaine Rouly by journalist Stéphane Bureau. Program Bien entendu. Radio-Canada Ici Première. December 23, 2019.
Interview of Serge Daneault with Dominique Lortie. Program: Un partenaire à votre santé [A partner for your health] (in French only). Radio VM. February 2021. Recording available online (in French only).
In collaboration with :


